In the modern digital economy, the most valuable commodity is no longer found in the earth, but within the encrypted servers of hospital systems and insurance providers. Medical records, once viewed as static administrative burdens, have been reimagined as high-octane fuel for the burgeoning artificial intelligence sector. However, as the race to dominate healthcare AI intensifies, a disturbing parallel has emerged between the world’s most sophisticated technology companies and the cyber-criminal syndicates that hold hospital systems for ransom. Both entities have identified the same truth: centralized health data is a gold mine, and the race to extract its value is outstripping the safeguards designed to protect it.
The current crisis is not merely a failure of security, but a fundamental flaw in the industry’s structural design. As Abhinav Shashank, CEO of Innovaccer, has pointedly observed, the perceived failures of AI in the medical space are often symptoms of a deeper ailment: healthcare’s outdated architecture. For decades, the industry has relied on centralized repositories of Private Health Information (PHI). While these silos were intended to streamline care, they have inadvertently created "honey pots" that are as attractive to silicon valley disruptors as they are to international ransomware groups.

The financial stakes of this data dependency were laid bare in February 2024, when Change Healthcare, a subsidiary of UnitedHealth Group, fell victim to a devastating ransomware attack. The breach, orchestrated by the ALPHV/BlackCat group, did more than just disrupt the American healthcare payment system; it resulted in a staggering $22 million ransom payment in Bitcoin. This was not an isolated incident but the culmination of a decade-long trend where healthcare has become the primary target for digital extortion. From a Los Angeles hospital paying $17,000 in 2016 to the multi-million dollar demands of today, the price of data recovery has skyrocketed.
Ironically, the same raw material that fuels these criminal enterprises is now being aggressively pursued by the world’s most powerful tech moguls. The launch of specialized tools like OpenAI’s ChatGPT Health and Anthropic’s Claude for Healthcare has triggered a frantic scramble among AI developers. These companies are desperate to train their Large Language Models (LLMs) on high-quality, longitudinal medical data. The difference between a ransomware group and a tech giant may lie in their legal standing and ultimate intent, but their dependency on centralized, vulnerable health records is identical. Both seek to monetize the most intimate details of human life—one through extortion, the other through algorithmic dominance.
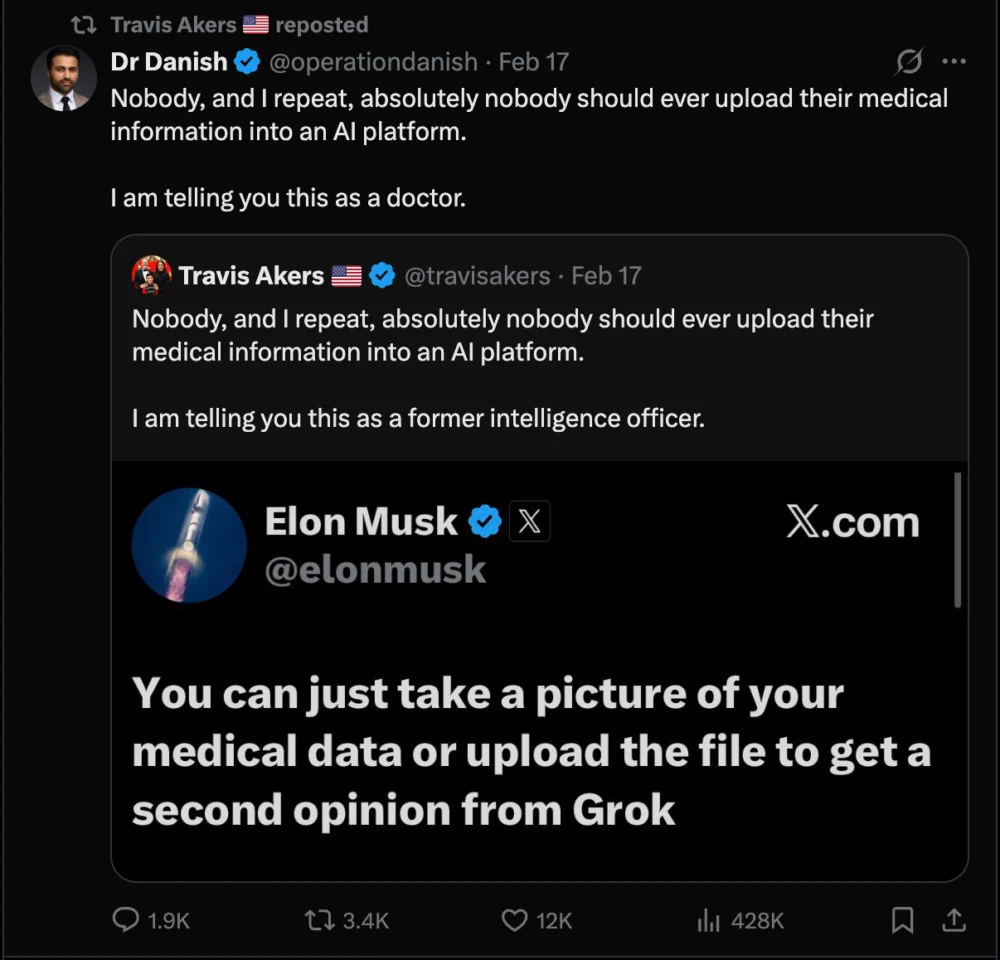
The tension between data utility and patient privacy reached a fever pitch recently when Elon Musk, owner of the X social media platform, encouraged users of his Grok AI to upload their medical records, including diagnostic imagery like X-rays and MRIs, to the platform. Musk’s proposition was framed as a way to improve the AI’s diagnostic capabilities, yet it was met with immediate and fierce resistance from the medical and intelligence communities. The suggestion highlighted a profound misunderstanding of—or perhaps a blatant disregard for—the regulatory and ethical frameworks that govern human health data.

Under the Health Insurance Portability and Accountability Act (HIPAA) in the United States, the protection of PHI is not a suggestion; it is a federal mandate. For an AI system to legally process PHI, it must be designated as a "Business Associate," a status that requires the signing of a Business Associate Agreement (BAA). This agreement binds the technology provider to strict standards regarding the storage, protection, and management of data under the HIPAA Security Rule. When a user uploads a medical record to a public AI model that lacks these protections, they are not just seeking a second opinion; they are potentially feeding their private history into a training set that may be used to develop future iterations of the model without their consent or any hope of "un-learning" the data.
This "AI gold rush" has raised alarms at the highest levels of global health governance. The World Health Organization (WHO) has warned that the rapid integration of AI into clinical settings is outpacing the development of safety standards. Dr. Essam Hamza, CEO of Rocket Doctor AI Inc., echoes these concerns, noting that many current systems rely on "opaque algorithms" and are prone to "hallucinations"—the phenomenon where an AI confidently asserts a factual falsehood. Without robust legal and clinical safeguards, these tools risk providing harmful advice to both patients and clinicians.
The danger of "silent trials"—where AI models are integrated into clinical workflows without rigorous, transparent testing—is a particular point of concern for researchers. Lana Tikhomirov, a PhD candidate at Adelaide University’s Australian Institute for Machine Learning, argues that global guidelines are desperately needed. If AI tools are rolled out prematurely, the unpredictable nature of these models could lead to catastrophic clinical outcomes. The challenge lies in the fact that healthcare AI is currently being built on a "move fast and break things" philosophy that is fundamentally incompatible with the "do no harm" oath of the medical profession.

To address these risks, a new school of thought is emerging among healthcare technology leaders. This approach advocates for a clear separation between the "presentation layer" of AI and the "clinical logic" of medicine. For example, Rocket Doctor AI utilizes LLMs solely as a way to interact with users, while ensuring that all differential diagnoses and recommendations are grounded in vetted, evidence-based medical knowledge developed by human clinicians over decades. By using AI as a support tool rather than a replacement for clinical judgment, the industry can harness the efficiency of automation without sacrificing the safety of the patient.
However, the question of "who benefits" remains the most contentious issue. Medical records are uniquely valuable because they are longitudinal, meaning they track a patient over a long period, and they are predictive. They don’t just record past illnesses; they can predict future disease risks, treatment adherence patterns, and even behavioral tendencies that correlate with purchasing power. When a tech company acquires this data for "free" through user uploads or opaque Terms of Service agreements, they are gaining an asset that has immense downstream financial value in the pharmaceutical, insurance, and advertising sectors.
The path forward requires a radical reimagining of data ownership. If health data is the fuel of the next generation of medicine, the patient must be the one who controls the pump. We are seeing the early stages of a movement toward "healthcare data wallets"—decentralized infrastructure that allows individuals to securely own and manage their own medical records. In this model, the patient grants temporary, audited access to a doctor or an AI tool, rather than the data being stored in a centralized server owned by a third party. This shift would simultaneously solve the "honey pot" problem for ransomware attackers and the "consent" problem for AI developers.

The transition to a patient-centric data model is not merely a technical challenge; it is a political and ethical one. The current architecture rewards centralization because it allows for easier monetization by those who control the silos. Shifting to a decentralized model requires overcoming the inertia of legacy systems and the lobbying power of entities that profit from the status quo. Yet, as the Change Healthcare attack demonstrated, the cost of maintaining the status quo is becoming unsustainable.
As we stand on the precipice of an AI-driven revolution in medicine, we must decide whether patients will be active participants in this new era or merely the "raw material" for it. The promise of AI—faster diagnoses, personalized treatment plans, and reduced administrative burdens—is real. But these benefits cannot be built on a foundation of data exploitation and structural vulnerability.
The next time a chatbot or a social media platform invites you to share your medical history for the sake of "innovation," it is worth pausing to consider the architecture behind the interface. In the digital age, your medical record is more than a file; it is a blueprint of your biological life. Protecting it requires more than just better encryption; it requires a fundamental shift in who owns the data, who profits from it, and who is ultimately responsible when the system fails. The gold rush is on, but the true value of healthcare data lies not in how it can be sold, but in how it can be used to safely and ethically improve human life.